News Story
Anthony Atala speaks at NC CEO Forum Healthcare Summit
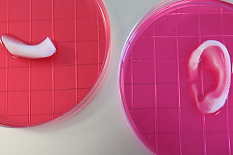
Creating transplantable organs in the lab, printing new cells on a burn victim’s body, and a body-on-a-chip may sound like scifi, but they’re all a reality at the Wake Forest Institute for Regenerative Medicine. So says Anthony Atala, MD, director of the institute, who spoke at the NC CEO Forum Heathcare Summit in Raleigh, Monday.
In his talk to the Forum and exclusive interview with WRAL Techwire, Atala described the scifi-like progress a the Institute (WFIRM) which he created at Wake Baptist after moving from Boston 14 years ago.
Scientists and doctors at WFIRM were the first in the world to engineer laboratory-grown organs and successfully implant them in humans. Currently, the 450-person Institute is working on more than 30 different replacement tissues and organs and developing healing cell therapies. Atala said 35 percent of the therapies are “in patients now.”
Atala noted that the first organ transplant occurred in 1954, but despite the many lives changed by this one accomplishment “we are still wrestling with challenges.” Those range from organ rejection to not enough organs for transplant. That is a problem that will only get worse at the population ages, he said. “The longer we live, the more potential there is for our organs to fail.”
A COMPLEX PROBLEM
So, he asked: “Can they be regenerated? Is that science fiction?”
Humans already regenerate our skin surface every two weeks, the cells in our bones every 10 years and in our brain every 20 years, he noted.
Regenerating human organs, however, is a problem that is increasingly complex depending upon the tissue, from skin cells to the major organs. The basic process used at the Institute is to take a small cell sample half the size of a postage stamp from a patient then expand and grow the cells in the lab before using them in therapy or to build a new organ such as a bladder.
In an interview, he compared the process of building a new organ with the cells on a scaffold to “a peanut butter and jelly sandwich” with the bread as the scaffold. “It’s much more complicated than that, of course,” he added.
The Institute has created therapies with skin, muscle, cartilage, kidney bladder, and vaginal tissues, among others.
PRINTING CELLS ONTO THE BODY
In the case of kidney disease, for instance, the patient’s cells are grown outside the body, mixed with a gell, processed and put back into the patient’s kidney weeks later. The treatment is in Phase II clinical trials in the US. A similar process allows regenerating muscle cells and blood vessels.
When scaffolds are used to build an organ such as a bladder, the material is made from the same used for stitches in surgery and degrades a few months later, but the new cells remain.
In another technology still under development, the Institute takes discarded organs, washes away the cells with a mild detergent, and two weeks later has something that looks like a liver and retains its blood vessel design, but without its cells. It is then perfused with liver cells.
“We can get them up to the size of a large lemon right now, but need to get them to the size of a football and we’re working on that right now,” Atala said.
They realized that making structures for therapy by hand one at a time would not work with larger numbers of patients and needed to scale the technology. So they developed a method to apply cells using, first, an ink jet printer, and then, a printer they designed themselves. The printer they designed uses a tiny nozzle 1/80th the size of a human hair that spits out the cells in a liquid that stiffens to a gelatin consistency right away.
“That gives us precision so we can put the cells where they are needed,” Atala said. He noted they can bring the latest version of their printer “right to the patient’s bedside.” The technology has been used to print new skin cells on burn victims.
BODY-ON-A-CHIP TESTS DRUGS
Another Institute technology has already resulted in the recall of a number of drugs. The body-on-a-chip technology they have engineered micro hearts, livers and lungs that can be used to test new drugs. By combining the micro-organs in a monitored system, the researchers aim to mimic how the human body responds to medications.
The goal is to help reduce the estimated $2 billion, 15-year slog to new drug development with its 90 percent failure rate.
“There is an urgent need for improved systems to accurately predict the effects of drugs, chemicals and biological agents on the human body,” said Atala.
The tiny 3D organs, called “organoids,” have already been used to detect toxicity in a handful of recalled drugs.
Atala said the Institute’s goal is to bring its therapies to more patients. Many are in late-stage clinical trials.
“Eventually we expect to demonstrate the utility of a body-on-a-chip system containing many of the key functional organs in the human body,” said Atala. “This system has the potential for advanced drug screening and also to be used in personalized medicine – to help predict an individual patient’s response to treatment.”
The Institute’s research is supported by a number of grants, including a $75 million grant from the Department of Defense.
Here’s a video on the WFIRM’s work.
Published February 14, 2018
















