News Story
Wake Forest Body-on-a-Chip Shows How Cancer Drugs Affect Organs

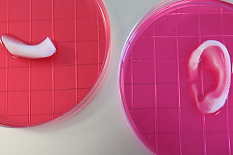
Wake Forest's body-on-a-chip system. The system consists of micro “organoid” versions of the heart, lung, and liver.
When pharmaceutical companies develop new medications, they face a 90 per cent failure rate. It sounds disheartening, but it’s really just part of the process for discovering what works and what doesn’t.
That high rate of failure, however, comes at a cost.
That’s because determining whether a new drug fails or succeeds requires a whole lot of investment—in the development of the pharmaceutical product in the first place, but also in the extensive testing equipment and live animal subjects needed to see how the drug performs.
The concept of the “body on a chip” could change all that. Scientists using advanced 3D bioprinting equipment are now able to fabricate human tissue made from real human stem cells. This means they can create scaled-down replicas of certain bodily organs that react in similar ways to their organic counterparts.
For Anthony Atala, M.D., director of WFIRM and senior researcher on a multi-institution “body on a chip” project, this progress has come not a day too soon. “There is an urgent need for improved systems to accurately predict the effects of drugs, chemicals, and biological agents on the human body,” he said, noting the cost and relative lack of accuracy involved in animal testing.
By creating a set of tiny 3D printed organs, or “organoids,” the WFIRM researchers have been able to develop a comprehensive platform for drug testing, allowing them to see how human organs react to drugs. They say it’s much more precise than cell screening and animal testing.
The system consists of a bioprinted heart and liver, with these organs being particularly vulnerable to the toxic effects of drugs. There are also miniature lungs in there to represent the point of entry for toxic particles and aerosol drugs like asthma inhalers.
The body on a chip is then monitored with a real-time camera, while a nutrient-filled liquid circulates through the system to keep the organoids alive.
This liquid also functions as the means of injecting drugs into the system.
Before any experimental therapies were pumped in there, the researchers first had to see how the system reacted to ordinary medications like painkillers. This, they explain, allows them to know if the organoids really behave like real organs.
"This system has the potential for advanced drug screening and also to be used in personalized medicine, to help predict an individual patient’s response to treatment."
Dr. Anthony Atala, Wake Forest Institute for Regenerative Medicine Director and CECT PI
“The data show a significant toxic response to the drug as well as mitigation by the treatment, accurately reflecting the responses seen in human patients,” said Aleks Skardal, the study’s lead author.
So far so good. But the biggest advantage of the body on a chip, the researchers say, is its ability to represent a drug’s effects on organs not directly targeted by the medication. For example, heart medicine could have an indirect effect on the liver, and this is something the system will help pick up on.
“If you screen a drug in livers only, for example, you’re never going to see a potential side effect to other organs,” said Skardal. “By using a multi-tissue organ-on-a-chip system, you can hopefully identify toxic side effects early in the drug development process, which could save lives as well as millions of dollars.”
This holistic approach to drug testing has already yielded some interesting results.
When the scientists subjected the system to a drug used to treat cancer, they found the drug to adversely affect the organoid heart. This was a surprise, since the researcher were only expecting to see consequences for the lungs, which can be scarred by the drug.
The WFIRM team thinks the drug moved inflammatory proteins from the lung to other organoids in the body on a chip, eventually causing the tiny heart to stop working.
“This was completely unexpected, but it’s the type of side effect that can be discovered with this system in the drug development pipeline,” Skardal said.
There’s more to come as well. In the near future, the scientists will upgrade the bioprinted system by increasing its speed and adding further 3D printed organoids.
“Eventually we expect to demonstrate the utility of a body-on-a-chip system containing many of the key functional organs in the human body,” said Atala. “This system has the potential for advanced drug screening and also to be used in personalized medicine, to help predict an individual patient’s response to treatment.”
The study, “Multi-tissue interactions in an integrated three-tissue organ-on-a-chip platform,” has been published in Scientific Reports.
Published November 7, 2017