News Story
New Smart Bandage Can Dispense Medication
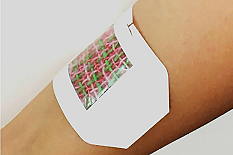
Experiments showed the smart bandage could regenerate skin tissue 3x faster than a standard bandage
Researchers from the University of Nebraska-Lincoln, Harvard Medical School and the Massachusetts Institute of Technology have designed a smart bandage that can simultaneously dispense medication.
The bandage is made of conductive fibers coated in gel, which can be filled with medications such as antibiotics or painkillers, according to Ali Tamayol, assistant professor of mechanical and materials engineering at UNL.
While it still acts as a regular bandage, the smart bandage features a stamp-sized microcontroller, which can be controlled by a smartphone or other wireless devices. This microcontroller sends voltage through the fibers of the bandage, heating and activating the medications in the gel.
Tamayol and his colleagues ran multiple experiments to evaluate potential advantages of the bandage. During one experiment, bandages loaded with growth factors were used on wounded mice. Over the same time frame, the smart bandage produced three times as much tissue compared to when a regular bandage was used.
Ali Khademhosseini, associate professor of health sciences and technology at Harvard University, is also a part of the research team.
“This technology is a game-changer, especially in common diseases like diabetes where diabetic ulcers are a consistent issue,” Khademhosseini said, noting the team’s vision of treating serious illnesses with the new technology.
The Centers for Disease Control and Prevention predicted triple the amount of diabetes cases in the United States by the year 2050. These cases often lead to chronic skin wounds, Tamayol said.
“The medical cost is huge for these cases, and there is a big need to find solutions for that,” Tamayol said.
The smart bandage could also be beneficial for the military or in cases where changing dressings for wounds is inconvenient or dangerous.
“We believe this technology can greatly reduce healthcare costs, decrease the need for repeated hospital visits and greatly improve patient outcomes,”
Ali Khademhosseini, CECT Collaborator
“Those wounded in combat could benefit from the bandage’s versatility and customizability,” Tamayol said.
The bandage could help stimulate faster healing of wounds, and medication within the dressing would prevent infection, Tamayol said.
Those in battle may suffer from numerous injuries and pathogens. The smart bandage’s potential lies in its variability to contain antidotes that target these hazards in what is possibly a remote environment, according to Tamayol.
The team has secured a patent for the smart bandage, but the product will still have to go through further animal testing and eventual human testing. The process could take up to several years before the smart bandage hits the market.
“We believe this technology can greatly reduce healthcare costs, decrease the need for repeated hospital visits and greatly improve patient outcomes,” Khademhosseini said.
As of now, most of the design’s components have been approved by the U.S. Food & Drug Administration, and this could streamline the process, Tamayol said.
The research team continues to work with the smart bandage, focusing on new advancements such as sensors that measure health-related indicators of skin tissue, such as pH and glucose levels. This integration could lead to the bandage being able to deliver proper treatments on its own.
For now, the smart bandage can accommodate multiple medications for a single wound. This level of customization and control can lead to faster healing, Tamayol said.
“This is a platform that can be applied to many different areas of biomedical engineering and medicine,” Tamayol said.
Read more at: http://www.dailynebraskan.com/news/new-smart-bandage-can-dispense-medication/article_b3b277f6-b3a7-11e7-8fc1-4762b516ae29.html
Published November 7, 2017